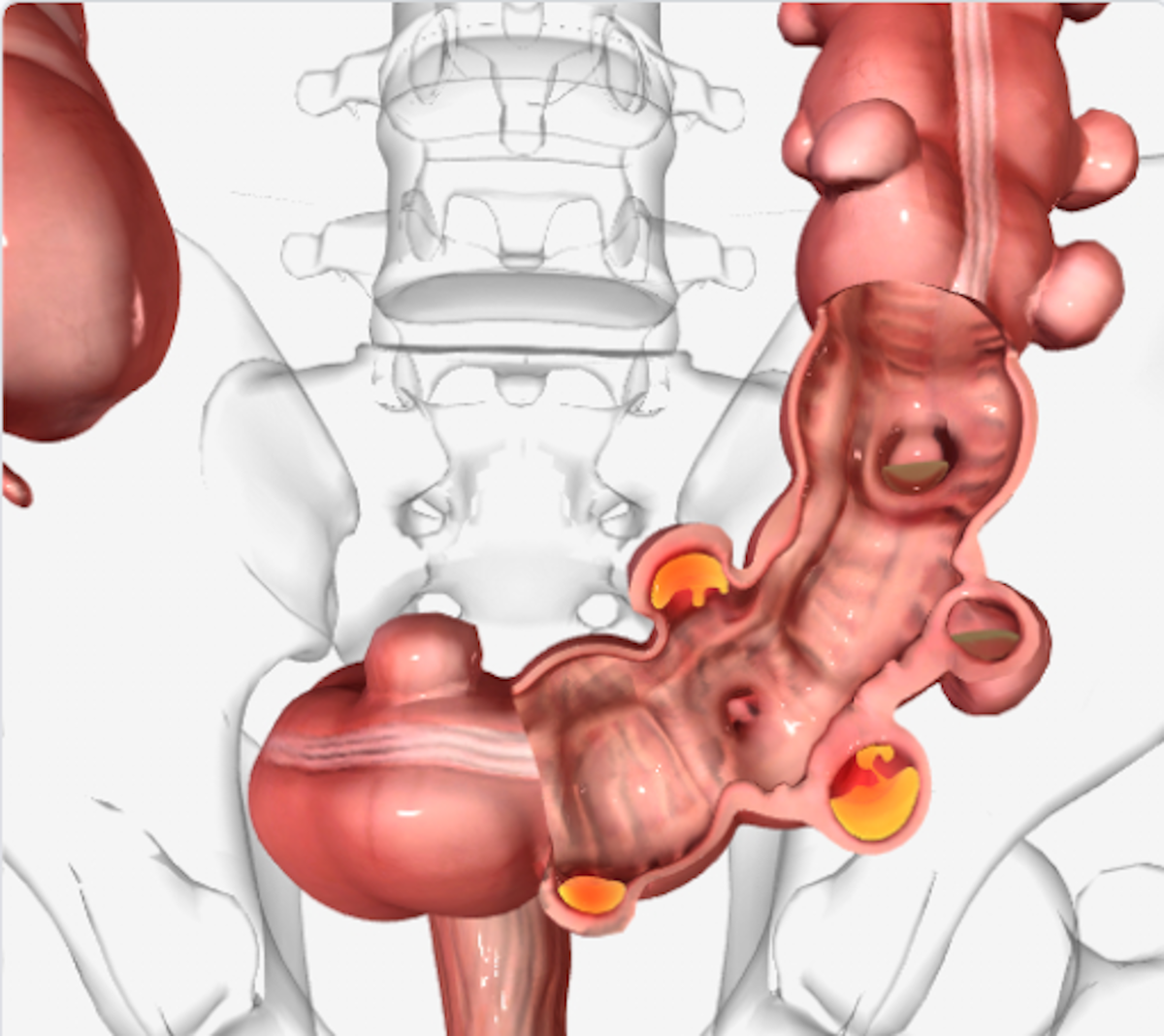
Diverticulitis is inflammation or infection of small pouches, called diverticula, which develop along the walls of your intestines. The pouches’ formation is a relatively benign condition known as diverticulitis. The pockets can form anywhere on the digestive tract. Still, they may develop at the end of the descending and sigmoid colons, and they also frequently occur on the first section of the small intestine, although problems are rarely found there.
Ageing and heredity are primary factors in the development of diverticulitis, but diet also plays a role. Eating a lot of low-fibre and refined foods can significantly increase the risk.
Treatment of diverticulitis
The British Journal of Clinical Practice says, “A high-fibre diet is effective in treating diverticulitis disease.” Research shows that fibre is essential for the prevention and treatment of diverticulitis.
Even when you have diverticulitis, you may not know it because the diverticula are usually painless and cause few symptoms. Sometimes, there are no symptoms. Sometimes, you may experience cramping on your left side that disappears when you pass gas or move your bowels. And, because diverticula will occasionally bleed, your stool may contain bright red blood.

Alkalising colonic irrigation with sodium bicarbonate
Safe and effective colon hydrotherapy includes an initial consultation. Consequently, sodium bicarbonate delivered to the colon through hydrotherapy can kill off candida.
You should consult your doctor if you have a fever, chills, abdominal swelling, or vomiting. The abdomen may become rigid, and movement causes pain. Blood may also appear in stools, indicating internal bleeding.
Diverticulitis
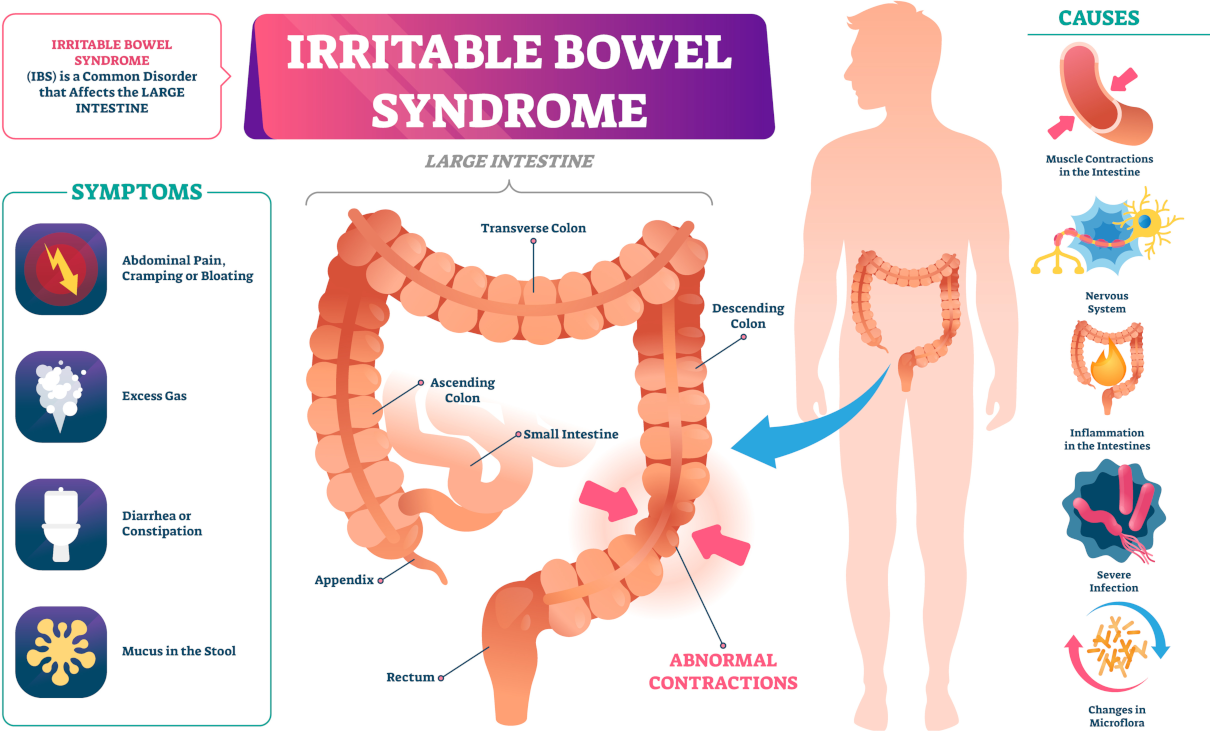
Diverticulitis occurs when the diverticula (sac-like, pea-sized protrusions in the intestinal wall) are inflamed. It typically forms if an individual suffers from frequent constipation, and eating a low-fibre diet may be a contributory factor. Diverticulitis can be either acute or chronic.
Symptoms
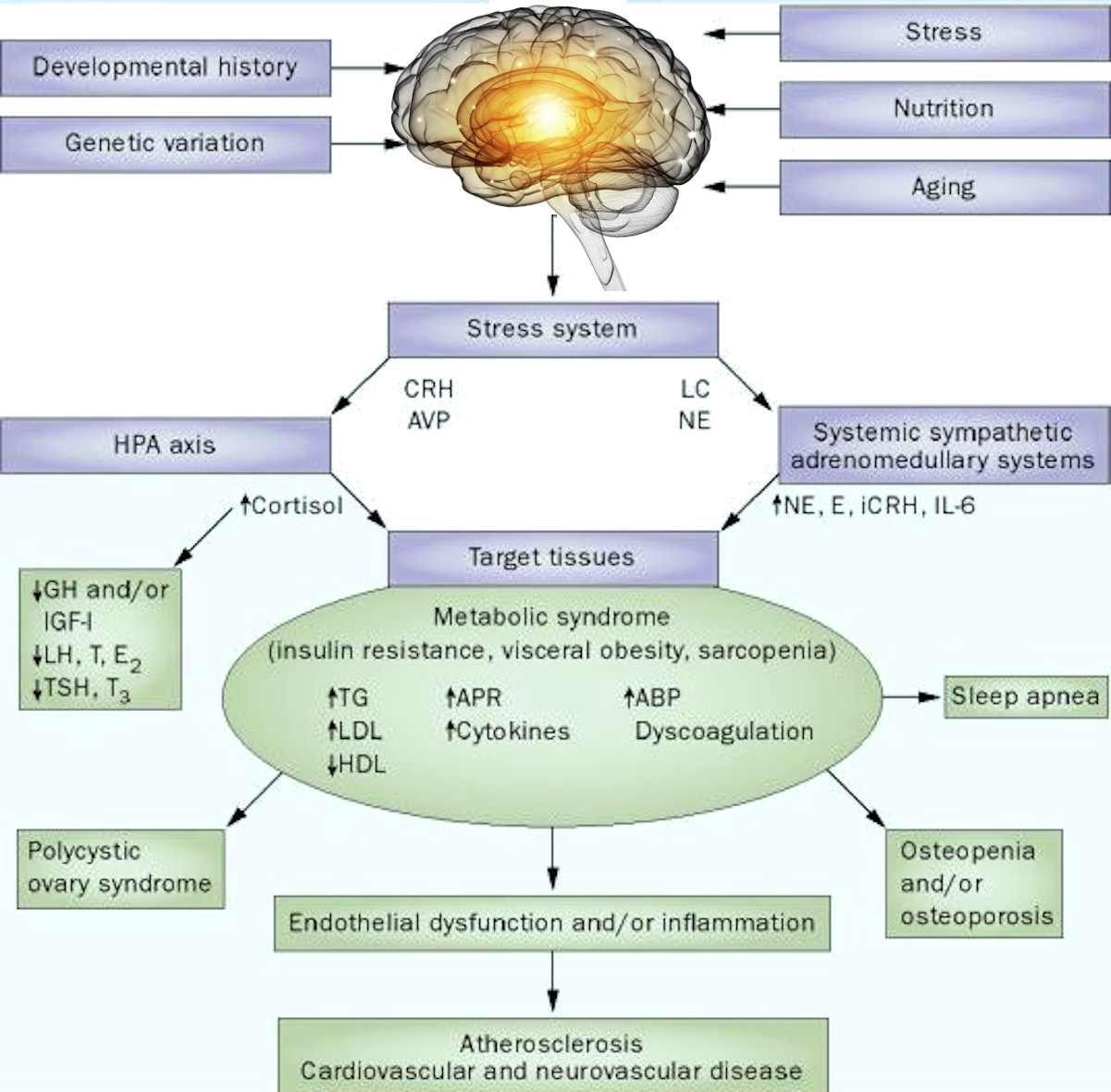
Symptoms include cramping, bloating, tenderness on the left side of the abdomen that is relieved by passing gas or a bowel movement, constipation or diarrhoea, nausea, and an almost continual need to eliminate. Because the large intestine walls often weaken as a person ages, this condition affects old rather than young people. Nobody knows what causes diverticulitis. However, we know that smoking and stress make symptoms worse. Poor eating habits compound the problem. A poor diet, a family history of the disease, gallbladder disease, obesity, and coronary artery disease increases the chances of diverticulitis. It is a classic example of a stress-related disorder.
Half arm waxing for women
Epilating women’s arms removes unwanted hair from the outside and inside of the arm. Experienced therapists using modern, high-quality materials will help you cope with your problem in our clinic.
Recommendations:
- The key to controlling this disorder is consuming adequate fibre and quality water. Drink at least eight 8-oz glasses of filtered water daily. Herbal teas, broth, and live juices can also contain some liquid. Liquid helps keep the pouch-like areas clean of toxic wastes, preventing inflammation.
- Eat a low-carbohydrate diet with high protein levels from vegetable sources and fish. However, do not eat grains, seeds, or nuts except well-cooked brown rice. These foods are hard to digest, resulting in bloating and gas. Also, avoid dairy, red meat, sugar, fried foods, spices, and processed foods.
- Eat plenty of leafy green vegetables. These are good sources of vitamin K. Obtaining this vitamin from the diet is especially important for people with intestinal disorders.
- Eat garlic for its healing and detoxifying properties.
Recommendations during an acute attack of diverticulitis:
- During a severe attack, your doctor may recommend a low-fibre diet temporarily. Once the inflammation clears, slowly switch back to a high-fibre diet.
- When an attack or pain begins, you may want to use a cleansing enema containing two quarts of warm water and the juice of a fresh lemon. It helps to rid the colon of undigested and entrapped food and relieve pain.
- On the day of an acute attack, take four charcoal tablets or capsules with a large glass of water (available at health food shops) to absorb trapped gas. Always take charcoal separately from medications and other supplements, and do not take it for prolonged periods, as it absorbs beneficial nutrients and gas!
- During severe attacks, use liquid or colloidal vitamin supplements for better assimilation. Blend all fruits and vegetables. Eat steamed vegetables only. Organic baby foods are best until healing is complete. Add psyllium to baby foods for gentle fibre. Drink “green” drinks (such as Udo’s Beyond Greens), carrots, and cabbage juices.
- Massage the left side of the abdomen to relieve pain. Stand up and do stretching exercises.
- DO NOT overuse laxatives; they can irritate the colon wall.

Signature facial
A facial bespoke of you, this treatment is result-driven and highly customized to each client. This facial treatment includes a deep cleansing, exfoliation, micro peel, extractions, serums, vitamin infusion, and masks. Depending on your skin’s need, over five advanced non-invasive modalities can be incorporated within the treatment, including a décolleté. Your skin condition and concerns will determine which one(s) would be suitable.
Considerations:
Food allergies/intolerances are often a cause of intestinal disorders. We advise Allergy testing.
Your doctor may recommend antibiotics. To replenish beneficial bacteria in the gut, consume organic plain yoghurt or probiotic supplements.
Supplements:
- Probiotics, beneficial bacteria (bio-Bifidus), are essential for replacing the flora in the small intestine, primarily to improve assimilation;
- Vitamin B complex – 100mg of each significant B vitamin thrice daily. It would be best if you had it for all enzyme systems in the body and proper digestion;
- Digestive enzyme complex – 1 with meals to break down proteins;
- Essential fatty acids – 1g of omega-3 fish oils three times a day; It improves lymphatic function and aids in protecting the cells lining the colon’s wall. It is also essential for reducing inflammation.
- Garlic – 2 capsules three times a day; It aids digestion and destroys unwanted bacteria and parasites.
- Take L-glutamine—500mg twice daily, on an empty stomach, with water or juice. Please do not take it with milk (it competes for protein digestion). This primary metabolic fuel for the intestinal cells maintains the villi (finger-like projections on the wall of the intestines through which nutrients are absorbed).
- Vitamin C – 2mg/3mg daily in divided doses; It reduces inflammation and boosts immune response.
- Chlorella

Food intolerance test of 208 ingredients
This is our most comprehensive food and drink test. It analyses your client’s IgG antibody reactions to 208 food and drink ingredients. This test will highlight their food triggers and help you formulate an IgG-guided elimination diet together.