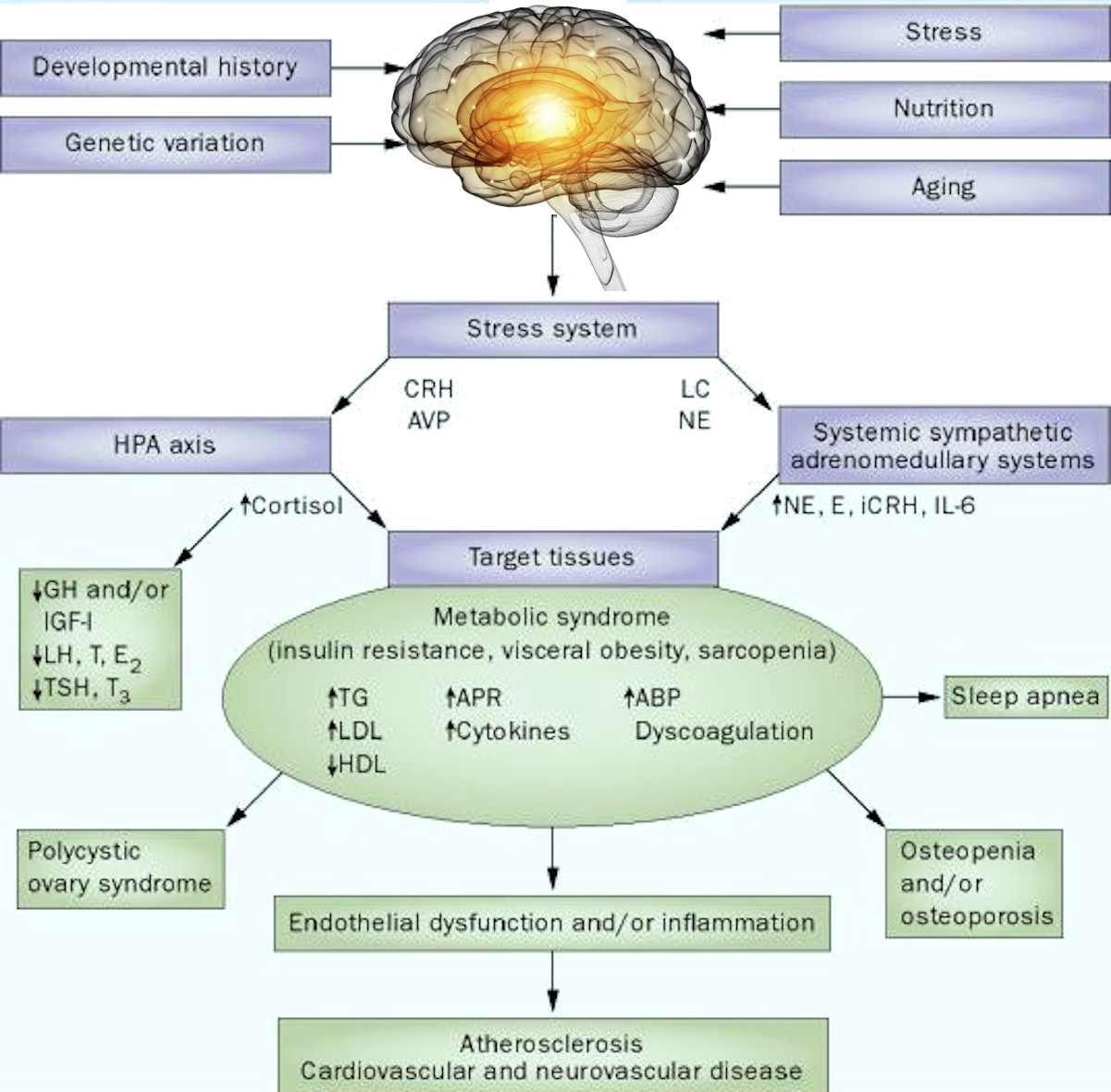
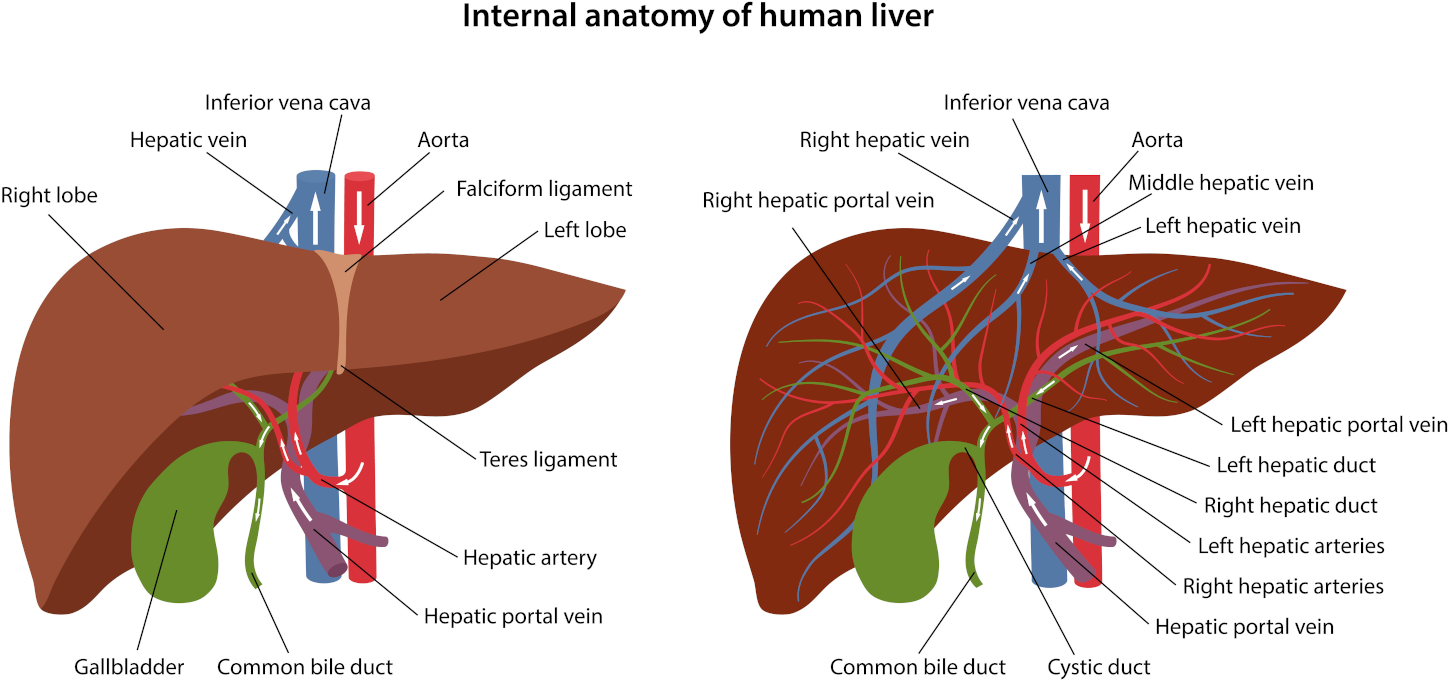
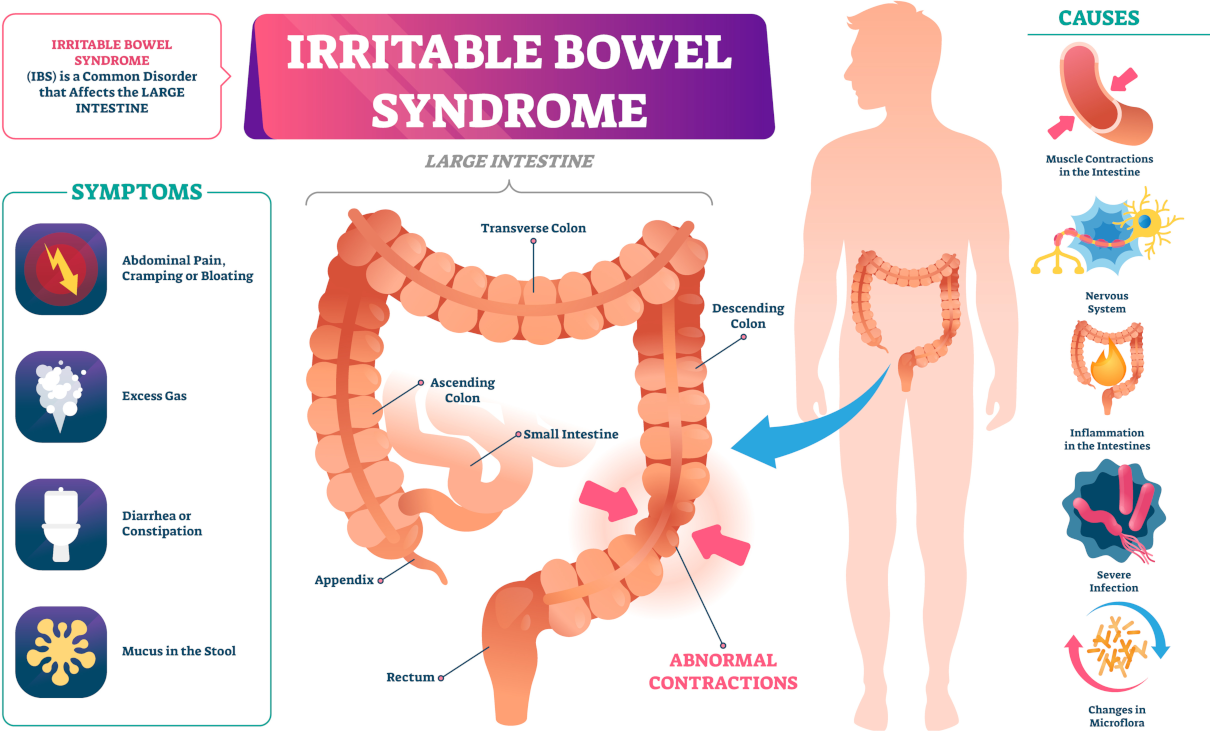
Intestinal bacteria (microbiota) affect human health and disease by regulating the immune system. It has become a fact of scientific and clinical significance. How does the intestine affect the immune system?
The intestinal microbiota profoundly affects the host’s immune system. Moreover, it depends on developing autoimmune diseases inside and outside the intestines. The question of how the guts affect the immune system worries many people. They want to maintain their health in excellent condition.
Besides genetic factors, environmental factors such as food and drugs are essential for the formation and composition of the intestinal microbiota. Constant consumption of unsaturated fats, carrageenan, and excessive use of antibiotics causes or significantly increases the risk of autoimmune diseases. It occurs through the use of immunomodulation mediated by intestinal bacteria. Therefore, we should treat these factors with extreme caution.
Probiotic implant and alkalising colonic with bicarbonate of soda
Alkalising colonic irrigation with bicarbonate of soda and high strength probiotic implants and comprehensive consultation is available at Parkland Natural Health Clinic.
Microflora
The microflora of the gastrointestinal tract (GIT) is closely related to the development and health of a person. Besides, it directly affects all aspects of the body’s vital activity. This fact underlies the question of how the intestine affects the immune system.
Scientific and technical achievements of recent years have allowed scientists to expand research methods significantly. Thanks to that, they gained a system-wide understanding of how a person’s immune system works. What is explicitly responsible for specific failures in the body?
How do bacteria and gut microorganisms in the intestine affect the immune system?
Different types of commensal intestinal bacteria promote specific differentiation of naive CD4 + T-cells, cells that have not yet entered into the recognition of foreign antigens. Immature CD4 + T cells can differentiate into four main cell types: Th1, Th2, Tregs and Th17. Differentiation of each line requires the induction of a transcription factor that is unique to each line. After differentiation, each line selects a unique set of cytokines. Th1 cells play an essential role in eliminating intracellular pathogens, while Th2 functions to combat parasitic infection.
The primary purpose of Th17 is to control the infection, and Tregs regulate the immune response.
One of the first review articles on the relationship between the immune system and human gastrointestinal bacteria was published in Science in 2006 by Metagenomic Analysis of the Human Distal Gut Microbiome.

Half leg & bikini line extended waxing
This waxing option is one of our London clinic’s most sought-after treatments. And this is primarily since the rhythm of the modern city makes us save time on hair removal on legs, spending thirty to forty minutes a month instead of devoting fifteen minutes of our precious time to shaving every day! 60 minutes
Affects the immune system.
Recent studies suggest that, in cases of certain diseases, the work of our immune system directly depends on the state of our gastrointestinal tract, the number and types of microorganisms that inhabit it and their interaction. The last article on nature.com discusses some research by scientists in this area: “Among the millions of bacteria that live in the intestines, scientists have discovered several species that play a principal role in keeping us healthy.”
The article, of course, does not fully cover the whole field of activity and the influence of the human microbiota on the state of the human body but gives a general idea of the strength and capabilities of the gastrointestinal tract bacteria.
In addition to confronting various diseases, the gastrointestinal microflora directly impacts the brain’s development and normal functioning. Attempts to kill the intestinal microflora lead to the suspension of the process of neurogenesis, the production of new cells by the brain. These are basic facts about how the intestine affects the immune system. To maintain a healthy microflora, it is necessary to undergo a colonic irrigation procedure periodically.

Mini Detox PLUS – 3 colonics, minerals, herbal & probiotic implants
The ideal pattern of colonic treatments includes three alkalising colon hydrotherapy treatments with sodium bicarbonate, one anti-parasitic implant on the first treatment, one liver and gall bladder stimulating herbal implant on the second treatment, and a high-strength probiotic implant on the third colonic.