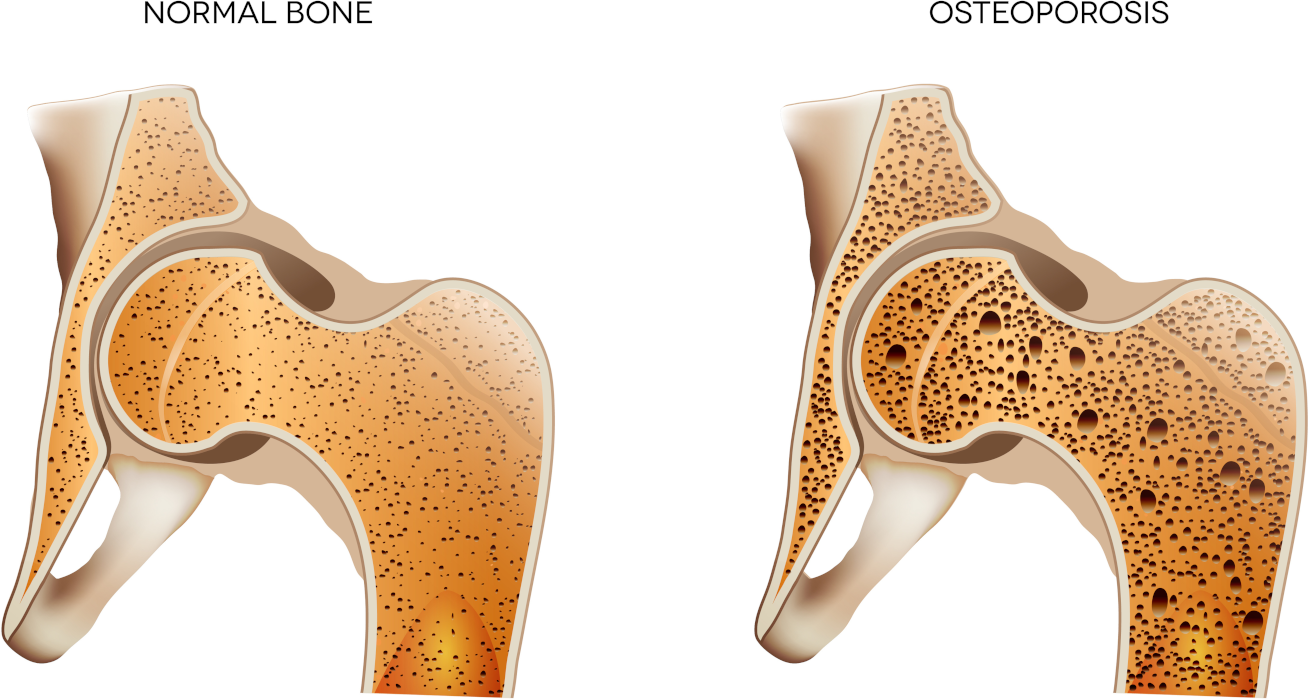
Osteoporosis, which means “porous bone,” is a progressive reduction in average bone mineral density, calcium mass, and strength, resulting in marked bone thinning and vulnerability to fracture. Although bone mass naturally declines by 1.5 – 2% per year in both sexes after age 40, women are at greater risk since their peak bone mass is naturally less than men’s due to their smaller size and muscle mass.
Osteoporosis is uncommon in men and is typically due to some underlying cause, such as long-term use of anti-convulsants or steroid drugs, alcoholism or thyroid problems. In women, osteoporosis is quite common, occurring in approximately one in four women after menopause and is due, in part, to the drop in progesterone and oestrogen. Both of which play essential roles in maintaining bone mass. Osteoporosis may affect the entire skeleton, but bone loss is usually most significant in the spine, hips, and ribs, as these bear a great deal of weight and are susceptible to pain, deformity or fracture.
Osteoporosis symptoms
Early symptoms:
- Usually none
- Backache
- Bone density test showing demineralisation of the spine and pelvis.
Late symptoms:
- Loss of height
- A deformed spinal column with humps
- Fractures, especially of the hip, arm and wrist, occur with a minor injury
- Severe backache
- Sudden back pain with a cracking sound indicating vertebral fracture
- Hip fracture

Initial osteopathic treatment and consultation
Find relief and restore balance with osteopathy at Parkland Natural Health. Initial osteopathic treatment with Gilly Arbuckle aims to reduce tension and restrictions, regain balance, and reduce pain or stiffness symptoms. The appointment includes a consultation and lasts forty minutes.
Causes
Men:
- Long-term use of steroids or anti-convulsant drugs
- Hyperthyroidism (overactive thyroid)
- Increased parathormone hormone levels
- Alcoholism
- Crohn’s disease
- Cystic fibrosis
- Hormonal deficiencies
Women:
- For calcium to be absorbed in the intestines, it must first be soluble and ionised by stomach acid. Thus, sufferers with insufficient stomach acid absorb only about 4% of an oral dose of calcium carbonate. However, it is the most widely utilised calcium for nutritional supplements. It is neither soluble nor ionised , even though people with standard stomach acid absorb only 22% of an oral dose of this calcium.
- The inability to convert vitamin D to its most active form stimulates the absorption of calcium, which our bodies produce.
- It lowers levels of oestrogen as well as progesterone after menopause. When oestrogen levels drop during the 3 to 5 years around menopause, the osteoclasts become more sensitive to the parathormone hormone. This hormone signals osteoclasts to increase their activity. Besides, the drop in oestrogen during menopause triggers the inflammatory mediator interleukin-6, which stimulates the growth of additional osteoclasts, thus increasing bone loss. Progesterone stimulates osteoblasts
- Lifestyle factors like coffee, alcohol and smoking cause a negative calcium balance. Thus, we lose more calcium than we take in. Lack of exercise, especially weight-bearing training, stimulates osteoblasts to build more bone. In contrast, inactivity doubles the rate of urinary and faecal calcium excretion. Lack of sun exposure , sunlight is the first step in the body’s production of the active vitamin D, which controls calcium absorption.

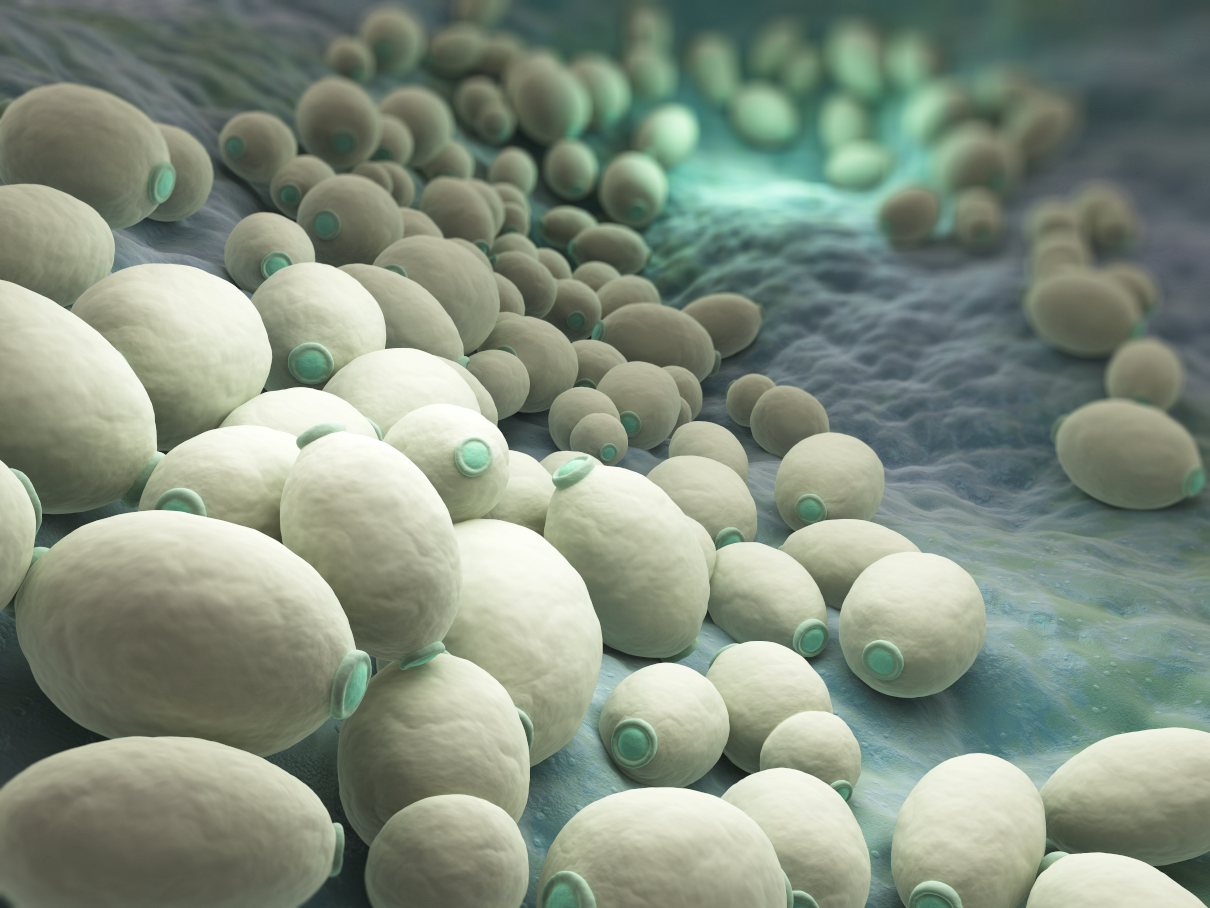
Anti-candida Mini Detox – three colonics with bicarbonate of soda
The Anti-candida mini detox involves a concentrated series of three colonics infused with bicarbonate of soda, ideally scheduled once weekly. This regimen serves as a potent initiation into a detoxifying cleansing routine, setting the pace for rejuvenation.
Diet for osteoporosis
Dietary factors include:
- Soft and fizzy drinks contain many phosphates and virtually no calcium. When phosphate levels are high, calcium levels are low as calcium is pulled out of the bones to balance things.
- High protein diets, these foods are acidic in the body. However, we need slightly alkaline body chemistry for good bone health.
- Refined sugar promotes acidic body chemistry. Following sugar intake, the urinary excretion of calcium increases.
- The intake of leafy green vegetables is inadequately low. However, they provide many vitamins and minerals necessary for bone health, including vitamin K and boron.
- Inadequate magnesium consumption occurs when magnesium levels are insufficient, and a decrease occurs in the active form of vitamin D. Also, we need magnesium to balance the hormones responsible for adequate calcium concentration levels in the blood.
- The consumption of vitamins B6, B12, and folic acid is inadequately low. Low levels of these vitamins lead to a build-up of homocysteine.
- Consumption of vitamin C is inadequately low. However, it is necessary for intercellular secretion of substances by all cells, including the formation of the osteoid by the osteoblasts.
Preventative measures
Preventative measures for osteoporosis:
- Go for regular weight-bearing exercise like jogging, trampoline, brisk walking, dancing, etc.
- Dont smoke
- Also, limit alcohol consumption to less than three servings per week.
- Don’t drink fizzy or soft drinks.
- Don’t drink more than two cups of coffee per day.
- Enjoy some sunshine to ensure vitamin D production. A 40-year-old woman should spend 10-15 minutes twice weekly in direct sunlight.
- Avoid processed foods. Their high salt and sugar content makes them the wrong choice for bone health.
- Consume a nutrient-dense, primarily vegetarian diet, rich in whole, unprocessed, preferably organic foods, mostly plant foods, and cold-water fish.

Food Intolerance Testing – Premium
Are you suffering from headaches, bloating, or tiredness? These are often signs of food sensitivity or intolerance affecting your daily life. Premium Food Intolerance Test is our most comprehensive food intolerance test, which analyses your IgG reactions to 208 food and drinks ingredients. YorkTest will provide precise results and nutritional support to help replace problem foods and optimise your diet.