Idiopathic hypertensia accounts for 90 per cent of all chronic hypertension cases. Today, 18-20 per cent of the adult population in economically developed countries suffer from hypertension. I.e. their arterial pressure repeatedly increases to 160/95 mm Hg and higher.
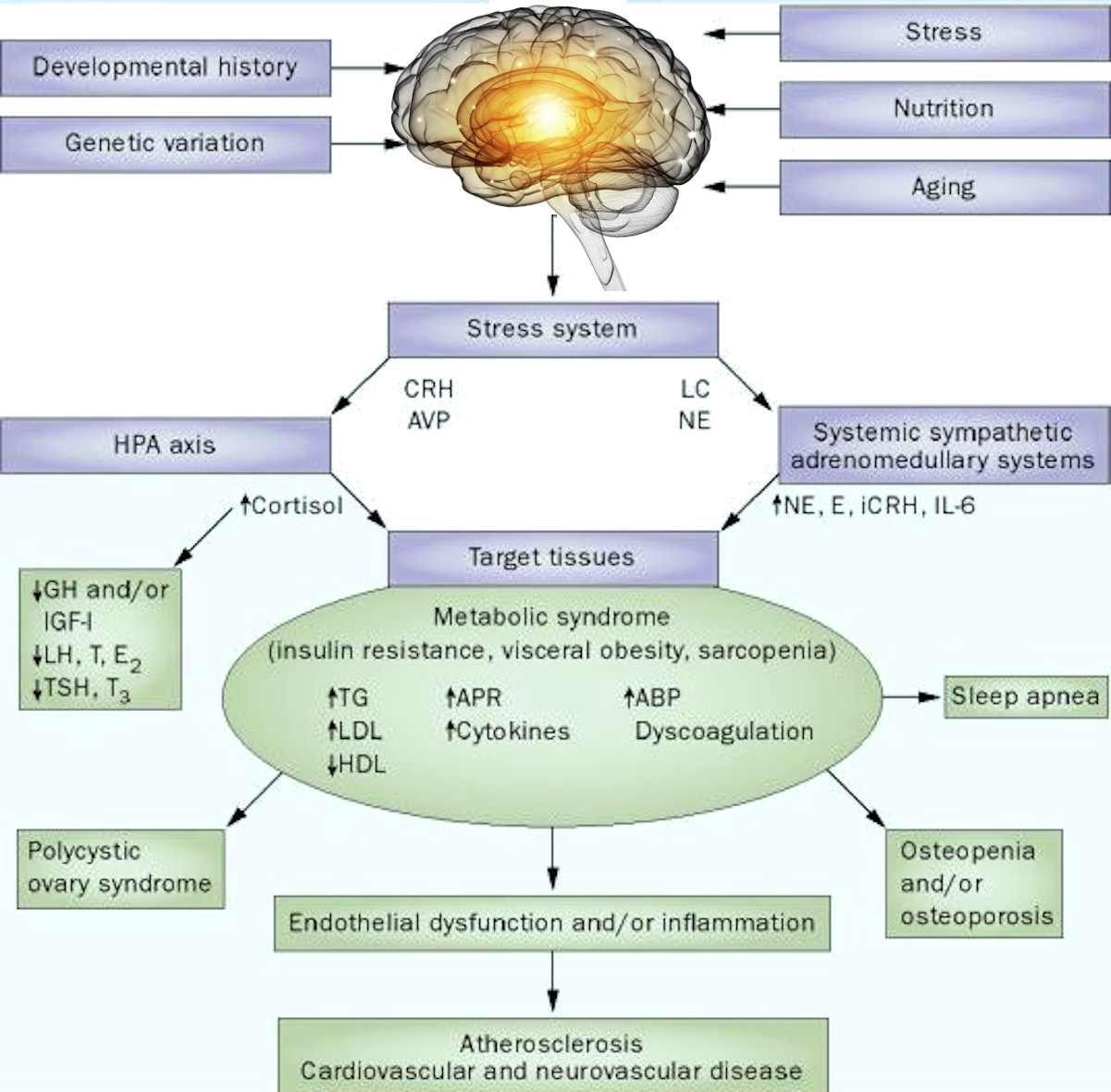
G.F. Langa’s theory on the decisive role of psychic overstrain and trauma in the development of hypertension says that noradrenaline, for instance, is an effector agent.
Expect
Idiopathic hypertensia will develop, providing some adverse external factors accompanying a hereditary predisposition. Besides, epidemiological research confirms that obesity and high arterial pressure are linked. The disease seldom affects people younger than 30 and older than 60. If a young man has steady systolodiastolic arterial pressure, there are good reasons to expect secondary, notably renovascular hypertension. As for people older than 60-65, high systolic pressure (160-170 mm Hg) given normal or reduced diastolic pressure usually deals with aorta atherosclerotic inspissation.

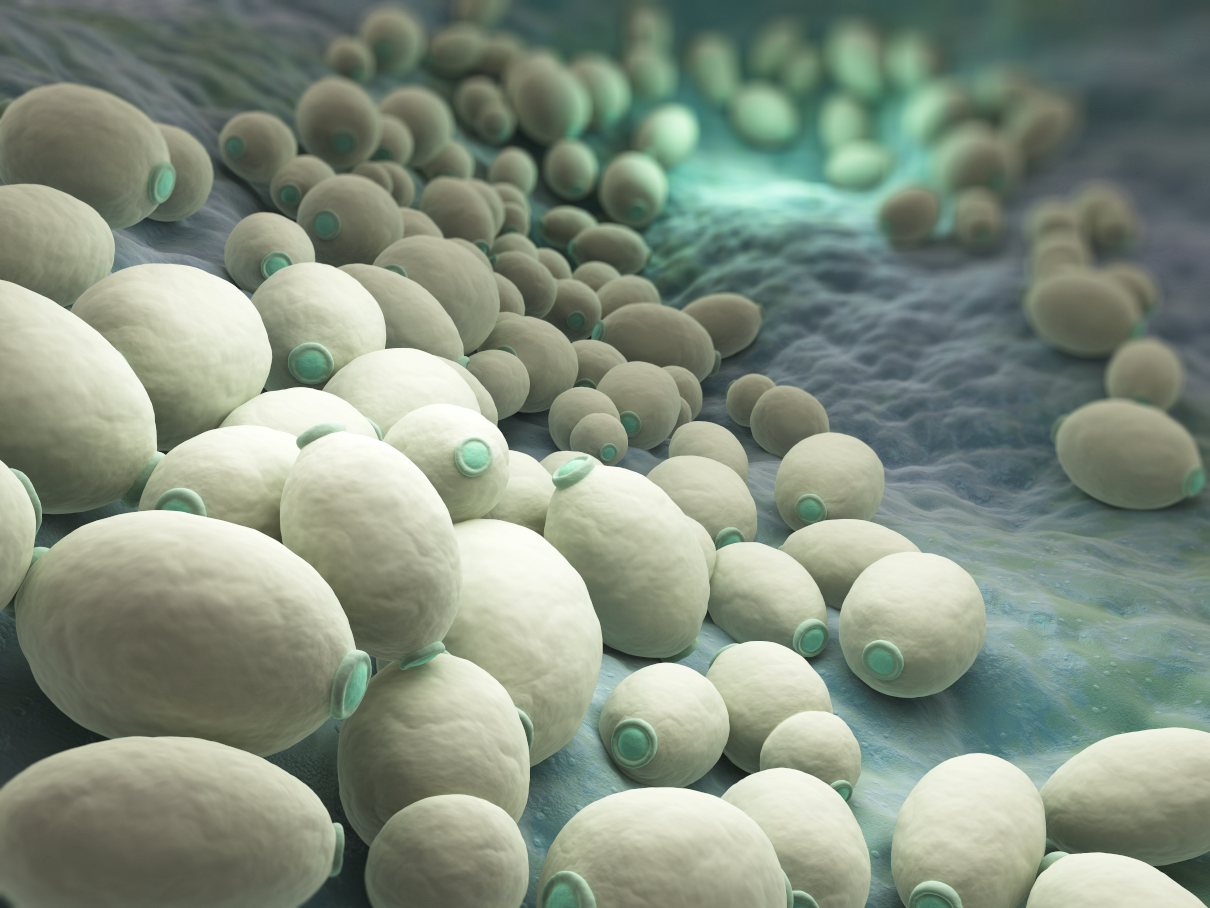
Anti-candida Mini Detox – three colonics with bicarbonate of soda
The Anti-candida mini detox involves a concentrated series of three colonics infused with bicarbonate of soda, ideally scheduled once weekly. This regimen serves as a potent initiation into a detoxifying cleansing routine, setting the pace for rejuvenation.
Progresses Idiopathic Hypertension
Hypertension progresses chronically and has periods of aggravation and remission. The disease may progress at a different pace. The condition can slowly become (benign) and rapidly move (malignant) under the hypertension classification used by the World Health Organisation (WHO). The slowly progressing form experiences three stages. Stage 1 (mild) is characterised by a relatively slight rise in arterial pressure, within 160-179 (180) mm Hg (systolic) and 95-104 (105) mm Hg (diastolic). The arterial pressure level is unstable when resting. It normalises gradually. Some patients feel normal, while others have headaches, head noises, insomnia, reduced mental efficiency, etc.
Patients may occasionally feel random dizziness and have nasal haemorrhages. The symptoms of the left ventricle’s hypertrophy are usually not observed. Stage 2 (moderate) features higher and more stable arterial pressure, which, when at rest, is within 180-200 mm Hg (systolic) and 105-114 mm Hg (diastolic). Patients often complain of headaches, dizziness and pain in the heart region, stenocardic in character. Hypertensive crises are typical of this stage.

Dermal Filler – Tear trough – dark circles
Dermal filler—Tear trough—Dark circles treatment with Teosyal Redensity II. One session may last up to sixty minutes. When booking your treatment online, you may add an extra syringe of a dermal filler to save fifty pounds.
Symptoms
Symptoms of the affection of the so-called target-organs become noticeable: hypertrophy of the left ventricle (sometimes only interventricular septa), weakening of the 1st tone at the apex of the heart and accented 2nd tone in the aorta. Besides, some ECGs show subendocardial ischemia. The central nervous system displays vascular insufficiency and transitional brain ischemia. So, brain insults are possible. As to the eye ground, the arterioles narrow, and the veins compress and expand. However, uroscopy shows no departure from the norm.
Arterial pressure amounts to 300 mm Hg (systolic) and 115-129 mm Hg (diastolic). Arterial pressure never normalises spontaneously. The clinical picture shows the affection of the heart (stenocardia, myocardial infarction, insufficient blood circulation and arrhythmia), brain (ischemic and hemorrhagic infarcts, encephalopathy), eyeground (angioretinopathy, type 2 and 3), kidneys (reduced renal bloodstream and glomerular filtration), etc. Some patients suffering from 3rd stage IDIOPATHIC HYPERTENSIA do not have severe vascular complications for years despite high and stable arterial pressure.

Food intolerance test of 208 ingredients
This is our most comprehensive food and drink test. It analyses your client’s IgG antibody reactions to 208 food and drink ingredients. This test will highlight their food triggers and help you formulate an IgG-guided elimination diet together.